COBRA vs ACA Marketplace: The $14,000 Mistake Early Retirees Make
You just left your job at 55. HR hands you a COBRA packet. It looks familiar — same doctors, same plan, same everything. You sign up because continuity feels safe.
That decision could cost you $14,000 or more in your first year alone.
Here is the math most early retirees never run before they choose.
What COBRA Actually Costs
Run your own numbers — FREE
10,000 Monte Carlo simulations. Forward-looking forecasts from BlackRock, JPMorgan, Vanguard, GMO, Schwab, Invesco. No account needed.
Try QuantCalc Free →COBRA lets you keep your employer health plan for up to 18 months. The catch: you pay the full premium — your share plus the portion your employer was covering — plus a 2% administrative fee.
Most employees only see their share of health insurance costs on their paycheck. The employer typically pays 70-83% of the premium. When you elect COBRA, you see the real number for the first time.
| Coverage Type | Average Monthly COBRA Cost (2026) | Annual Cost |
|---|---|---|
| Individual (age 55-64) | $823 | $9,876 |
| Individual (PPO, major metro) | $1,100-$1,400 | $13,200-$16,800 |
| Couple (both 55-64) | $1,646 | $19,752 |
| Family | $2,100+ | $25,200+ |
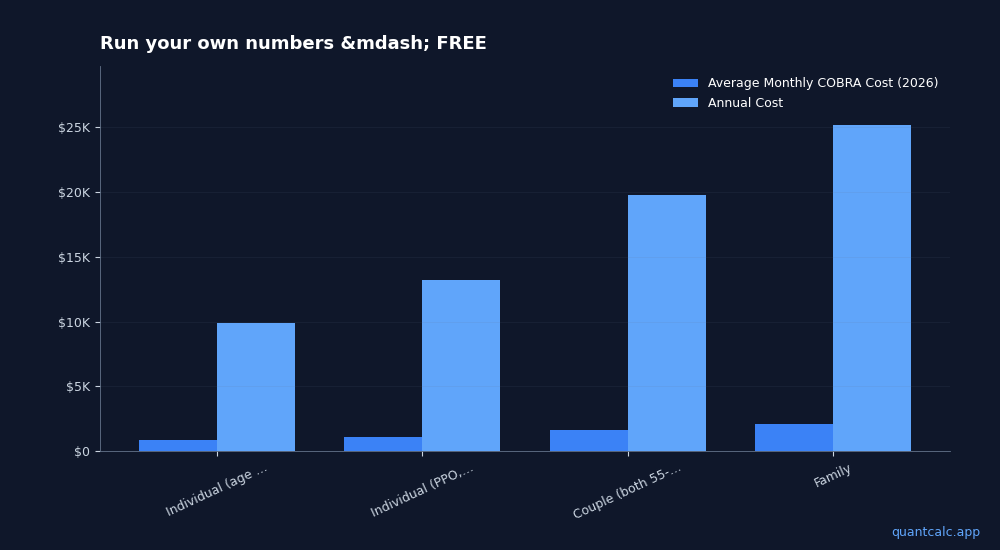
Source: KFF 2025 Employer Health Benefits Survey extrapolated to 2026 with 7% premium inflation. COBRA adds 2% admin fee on top.
Those numbers are not subsidized. COBRA premiums receive zero federal premium tax credits. You pay the full amount regardless of your income.
What ACA Marketplace Plans Cost With Subsidies
ACA Marketplace plans are a different calculation entirely. Your premium depends on your income — specifically your Modified Adjusted Gross Income (MAGI).
For an early retiree whose only income is investment withdrawals and maybe some part-time consulting, MAGI can be remarkably low. And low MAGI means large premium tax credits.
Here is what a 60-year-old single person in a mid-cost state pays monthly for a Silver plan at different income levels in 2026:
| Household MAGI | Monthly Premium (Silver) | Annual Premium | Annual Savings vs COBRA ($1,100/mo) |
|---|---|---|---|
| $20,000 | $0-$50 | $0-$600 | $12,600+ |
| $35,000 | $120-$200 | $1,440-$2,400 | $10,800-$11,760 |
| $50,000 | $350-$450 | $4,200-$5,400 | $7,800-$9,000 |
| $60,000 | $500-$600 | $6,000-$7,200 | $6,000-$7,200 |
| $62,600 (at the cliff) | $500-$600 | $6,000-$7,200 | $6,000-$7,200 |
| $64,000 (over the cliff) | $1,100-$1,300 | $13,200-$15,600 | $0 or WORSE |
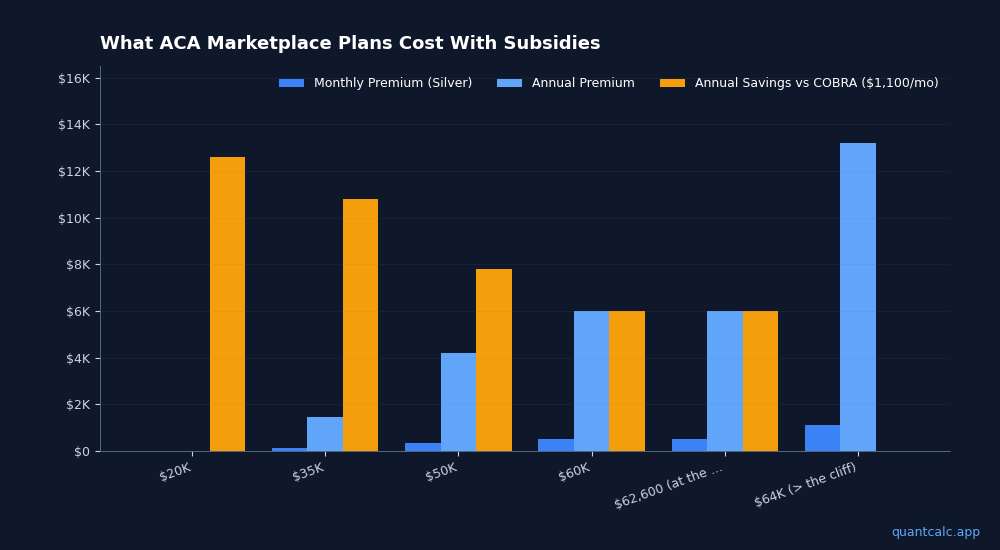
That last row is the number that wrecks early retirement healthcare plans.
The 400% FPL Cliff Changes Everything
In 2026, the enhanced ACA premium tax credits expired. The 400% Federal Poverty Level cliff is back. For a single person, the cliff sits at $62,600. For a couple, $84,640.
Earn $62,500 and you might pay $500/month for a Silver plan. Earn $64,000 — just $1,500 more — and you could owe $1,300/month because the premium tax credit disappears entirely.
That single dollar difference translates to roughly $8,700 per year in lost subsidies.
This is why the COBRA vs Marketplace decision is not just about comparing sticker prices. It is about whether you can control your income precisely enough to stay below the cliff.
When COBRA Actually Makes Sense
COBRA is the right choice in a narrow set of situations:
1. You are mid-treatment. If you are in the middle of chemotherapy, a pregnancy, or a complex surgical recovery, switching plans and potentially switching provider networks mid-treatment carries real risk. COBRA preserves your exact network for 18 months.
2. Your income will be too high for subsidies anyway. If you are taking a large severance payout, exercising stock options, or doing a major Roth conversion in your first retirement year, your MAGI may blow past the 400% FPL cliff regardless. In that case, the ACA Marketplace premium without subsidies may be comparable to COBRA.
3. You need a very short bridge. If you are 63.5 years old and Medicare kicks in at 65, an 18-month COBRA bridge might cost less in total hassle than setting up a Marketplace plan for one year.
Outside those scenarios, the ACA Marketplace wins on cost for most early retirees.
The MAGI Management Strategy That Saves Thousands
The real power of ACA Marketplace plans is that you get to engineer your income. Unlike W-2 employment, early retirement gives you unprecedented control over MAGI.
Here is how smart early retirees keep MAGI below the cliff:
Withdraw from Roth accounts first. Roth IRA and Roth 401(k) withdrawals do not count as MAGI. A retiree living on $80,000/year can withdraw $40,000 from Roth accounts and only report $40,000 of MAGI — well below the cliff.
Time your Roth conversions carefully. A Roth conversion ladder is essential for early retirees, but each conversion dollar adds to MAGI. Convert too aggressively in a year when you need ACA subsidies, and you push yourself over the cliff.
Harvest capital gains strategically. Long-term capital gains count as MAGI. Selling $30,000 of appreciated stock might save you 0% in federal capital gains tax if your total income is low enough, but it could simultaneously push you over the ACA cliff and cost you $8,700 in lost healthcare subsidies.
Manage the timing of consulting or freelance income. If you do part-time work in early retirement, billing $5,000 in December vs January can make the difference between keeping and losing subsidies for an entire year.
This is where generic retirement calculators fail. They model healthcare as a fixed annual cost. They do not model the interaction between Roth conversions, capital gains, ACA cliff thresholds, and the actual premium you will pay. You need a calculator that stress-tests your MAGI against the cliff across thousands of scenarios.
The 60-Day Window You Cannot Miss
When you leave your job, you trigger a Special Enrollment Period (SEP) for the ACA Marketplace. You have 60 days from your last day of employer coverage to enroll. Miss this window and you wait until Open Enrollment (November 1 - January 15).
One important nuance: you can elect COBRA retroactively within 60 days of losing coverage. This creates a strategic option. If you get sick in month one after leaving your job, you can retroactively elect COBRA to cover those expenses, then let COBRA lapse and switch to the Marketplace.
However, the 60-day SEP for the Marketplace starts when your employer coverage ends — not when COBRA ends. So if you elect COBRA first, your Marketplace SEP may have already expired by the time COBRA runs out. Plan the sequence carefully.
The Real Math: A Case Study
Sarah, age 58, leaves her corporate job. Her situation:
- COBRA premium: $1,150/month ($13,800/year)
- Retirement income (dividends + part-time consulting): $48,000 MAGI
- 400% FPL for single person: $62,600
Option A — COBRA: $13,800/year. No subsidies. No MAGI management needed.
Option B — ACA Marketplace Silver: At $48,000 MAGI, her premium is roughly $380/month ($4,560/year). She also qualifies for cost-sharing reductions on a Silver plan, lowering her deductible and copays.
Annual savings: $9,240. Over the 3-7 years until Medicare at 65, that is $27,720 to $64,680 kept in her portfolio compounding — money that makes her retirement significantly more secure.
But here is the trap: Sarah also wants to do a $20,000 Roth conversion each year. That pushes her MAGI to $68,000 — over the cliff. Suddenly her ACA premium jumps to $1,200/month and the Marketplace costs MORE than COBRA.
The solution: convert only $14,500 to stay at $62,500 MAGI. She leaves $5,500 of conversion on the table but saves $8,700+ in healthcare subsidies. Net benefit: still $3,200 ahead.
This is the kind of tax-healthcare interaction that breaks simple spreadsheet models.
Run Your Own Numbers
The COBRA vs Marketplace decision depends entirely on your specific MAGI, age, state, and family size. There is no universal answer — only your answer, stress-tested against different income scenarios.
QuantCalc's free ACA Cliff Calculator models the exact subsidy cliff threshold for your household, shows how Roth conversions and capital gains affect your premium, and stress-tests your MAGI across multiple scenarios. See what happens to your healthcare costs before you sign the COBRA paperwork.
Frequently Asked Questions
Can I switch from COBRA to the ACA Marketplace?
Yes. Losing COBRA coverage (or exhausting COBRA) triggers a new 60-day Special Enrollment Period for the Marketplace. However, voluntarily dropping COBRA may not always trigger a SEP in every state. The safest path: let COBRA expire naturally, or enroll in the Marketplace during your initial 60-day SEP when you first leave your job.
Does COBRA coverage count toward the individual mandate?
Yes. COBRA is qualifying health coverage under the ACA. In states that still enforce an individual mandate (California, Massachusetts, New Jersey, Rhode Island, DC), COBRA satisfies the requirement.
What if my income changes mid-year?
ACA subsidies are reconciled on your tax return. If your income ends up higher than estimated, you repay excess subsidies. If lower, you get additional credit. COBRA has no income-based adjustment — the cost is fixed regardless.
Is COBRA worth it just for the first month while I set up Marketplace coverage?
Usually not. Marketplace coverage can start the first of the month following enrollment. COBRA retroactive election is a better short-term hedge — if nothing happens in month one, you never elect COBRA and never pay for it.
QuantCalc is an independent educational tool. Not affiliated with, endorsed by, or sponsored by any referenced firm including BlackRock, J.P. Morgan, Vanguard, GMO, Schwab, Invesco, Morningstar, or Fidelity. Return assumptions derived from publicly available research. All trademarks belong to their respective owners. Not financial advice.
Frequently Asked Questions
Yes. Losing COBRA coverage (or exhausting COBRA) triggers a new 60-day Special Enrollment Period for the Marketplace. However, voluntarily dropping COBRA may not always trigger a SEP in every state. The safest path: let COBRA expire naturally, or enroll in the Marketplace during your initial 60-day SEP when you first leave your job.
Yes. COBRA is qualifying health coverage under the ACA. In states that still enforce an individual mandate (California, Massachusetts, New Jersey, Rhode Island, DC), COBRA satisfies the requirement.
ACA subsidies are reconciled on your tax return. If your income ends up higher than estimated, you repay excess subsidies. If lower, you get additional credit. COBRA has no income-based adjustment — the cost is fixed regardless.
Usually not. Marketplace coverage can start the first of the month following enrollment. COBRA retroactive election is a better short-term hedge — if nothing happens in month one, you never elect COBRA and never pay for it. QuantCalc is an independent educational tool. Not affiliated with, endorsed by, or sponsored by any referenced firm including BlackRock, J.P. Morgan, Vanguard, GMO, Schwab, Invesco, Morningstar, or Fidelity. Return assumptions derived from publicly available research. All trademarks belong to their respective owners. Not financial advice.